What is Wound Dehiscence?
When a surgical wound heals properly, the sutures around its edges stay intact while new tissue, known as “granulation tissue,” starts forming. One of the most common complications of surgical wounds is when the surgical incision breaks along the suture. In other words, the wound splits open, a condition known as wound dehiscence.
Why does wound dehiscence occur?
Wound dehiscence is caused by many things such as age, diabetes, infection, obesity, smoking, and inadequate nutrition. Activities like straining, lifting, laughing, coughing, and sneezing can create increased pressure to wounds, causing them to split. Chronic use of corticosteroids (steroid hormones made in the adrenal cortex or synthetically), previous scarring, the presence of radiation at the incision site, improper stitch usage, unsuitable suture type, fluid-coagulant balance, cancer, and surgical errors can also contribute to wound dehiscence.
Dehiscence can also occur due to poor wound undermining throughout the surgery. Wound undermining means that damaged tissue extends under the skin and can’t be seen on the surface.
The location of the wound can also cause dehiscence. For example, wounds located on the legs, shoulders or back, or in mobile areas or areas prone to high tension, are at increased risk of rupturing.
Patients diagnosed with Ehlers-Danlos syndrome are more likely to experience dehiscence. Ehlers-Danlos syndrome is an inherited disorder that affects connective tissue, particularly skin, joints and blood vessel walls.
Symptoms of wound dehiscence
Some common symptoms of dehiscence are:
- Broken sutures that don’t heal.
- Bleeding from wound and bleeds at the surgical wound entry points.
- Fever.
- Inflammation.
- Pain at the wound site with high sensitivity to touch.
- Sudden opening of the wound.
- Swelling.
- Wound drainage – pus-filled and frothy.
A frequent effect of wound dehiscence is arterial bleeding. Blood from an arterial bleed is brighter in color and may spurt, or pulsate. Arterial bleeds occur more often in patients who are overweight or suffering from diabetes.
Causes of wound dehiscence
One of the leading causes of wound dehiscence is infection. Some characteristic signs of infection are:
- Abscess – swollen area that contains pus.
- Erythema – abnormal redness of the skin.
- High body temperature.
- Large amounts of exudates – seepage from the wound area.
- Odor.
- Severe pain.
How is wound dehiscence treated?
Dehisced wounds require immediate attention. After the wound is sutured closed, doctors primarily use one of two methods to treat dehiscence.
- Antibiotics – Use of an antibiotic ointment over a newly sealed wound may prevent any possible future infections.
- Debridement – Removal of any dead or damaged tissue from the surgical wound. Doing so creates a better seal for a new surgical closing. It can also improve the development of healthy skin tissue.
If a wound has previously suffered a dehiscence, it must be monitored closely. Careful observation minimizes any issues that may occur during this second healing process.
13 possible reasons for wound dehiscence
Although there are many reasons that contribute to wound dehiscence, what follows are the most common.
Utilization of inappropriate knot
The importance of proper suture knot techniques
When it comes to suturing, knots are much more than tying off the ends of materials passed through body tissues. Maintaining appropriate tension on the suture is vital to healing, so knots have to be set properly to ensure stitches remain intact.
Surgeons determine what type of knot to use when closing wounds. In the picture below [1], from left to right, are three frequently used:
- Simple knot – incomplete basic unit
- Square knot – completed common knot
- Surgeon’s or friction knot – completing tension

How suture material and suture experience affect knots
The knotting technique used depends mainly on the nature of suturing material. For example, multifilament materials are those that are made by braiding or twisting so that the coefficient of friction rate is high. As a result, knots hold well and remain tied as they are created. Monofilament materials consist of only one strand of fiber, and their coefficient of friction rates are much lower meaning that they tend to come untied more easily. Also, synthetic polymeric monofilament suture materials have “memory” which means they tend to return to their original shape instead of lying flat, which is a desired quality in suturing.
The quality of suture knots is also a product of the skill of the person applying them. The positioning of knots is determined by the suture technique and wound being treated. These decisions determine how secure the knot remains. Using the wrong knots or tying them too hastily compromises knot quality.
Potential problems caused by improper suture knots
Proper suture knots are vital to the overall suturing process to ensure that wounds heal effectively.
Improper suture knotting techniques can cause the knots to loosen or come undone entirely. This, in turn, relieves the holding tension of the suture, allowing the wound to open. An open wound will not heal correctly, causing infection or excessive scarring. Incorrect knotting techniques can also leave too much material remaining which not only becomes a snag hazard but can produce more significant irritation and discomfort to the patient.
Knowing which suturing knot technique is appropriate is essential since the primary focus of wound suturing is to create closure for the wound. When suturing is done correctly, it reduces bacterial entry, heals properly, and produces the least scarring possible.
Tying knots too loosely
If suture knots are applied too loosely, they can allow the suture to slip and lose tension. Loose knots snag easily during daily activities which can cause the stitch to break, increasing the possibility of the wound opening. If a suture is not held under its ideal tension by a correctly tied knot, the healing properties of the wound will be compromised. This can lead to improper healing, and bacteria may enter the wound creating infection, excessive scarring, and greater discomfort.
Sutures and knots can become loose even when they have been applied properly. The objective is to repair the suture before any lasting damage occurs to the wound. Suture tension must be regained to keep the wound closed, allow for full healing, resist infection, and minimize discomfort and scarring.
Employment of improper suture material
Heavier suture materials provide the best tension strength for holding wounds closed, and require fewer and more secure knots. Lighter materials cause less tissue irritation and damage and glide through wounds more efficiently. But they need several knots for adequate closure. Thin suture materials, therefore, are selected for cosmetic areas, such as the face, to produce less scarring. If a thick suture material is used on the face, more noticeable wound and suture track scars are the results.
Also, using absorbable versus non-absorbable or braided versus non-braided suturing materials incorrectly can lead to problems. Absorbable materials dissipate over time and do not require removal. Such materials can be somewhat unpredictable in their breakdown which, if used on surface wounds, can occur early leaving them prone to opening or tearing.
The choice between using braided or non-braided sutures is just as important. Braided materials are woven together and provide better knots and wound tension, but are also considered causes of more adverse skin reaction. Additional, they can present a higher risk for infection due to the presence of grooves where germs can enter the wound.
Selection of the incorrect needle
One of several types of needles can be selected for the suturing process. Two primary ones are cutting needles and round body needles.
Cutting Needles – Cutting needles have two sharpened point edges that oppose one another. This design is for use on dermal tissue that is tough and difficult to penetrate, such as dense, thick and irregular connective tissue. Variations include conventional cutting needles and reverse cutting needles. Traditional cutting needles have a three-blade, triangular-shaped tip that is sharpened on the inner convex for better penetration and a flattened body which is more easily grasped by a needle holder. Reverse cutting needles have sharpened edges on the outer convex and are used to suture extremely tough yet delicate dermal tissue such as oral mucosa and tendon sheath.
Round Body Needles – These suture needles have a tapered, sharpened tip and a round body designed to pierce instead of cut skin tissue. The grasping end is rectangular or oval for better holder control. Round body needles are used in soft, easily penetrable tissue, such as subcutaneous layers, abdominal viscera, peritoneum, myocardium tissue, etc.
Cutting needles cause less injury to tough types of tissue because it will penetrate the tissue with minimal force as opposed round body needles where excessive force is needed to penetrate the tissue – but it may actually cause more damage in softer tissue like fascia – by tearing through the tissue causing damage and scarring. When this happens, it may indirectly increase the risk of infection.
Some bodily structures are quite thin and friable, so always remember a cutting needle can cut through the tissue like a scalpel. Consider using a reverse cutting needle in certain situations.
Over-tightening of sutures
The importance of not suturing wounds under tension is emphasized in most surgical skills and suturing courses. Excessive pressure may cause the suture to break and could cut tissue which leads to the wound opening. Practice in avoiding too much tension leads to the successful use of finer gauge materials.
The following case study illustrates what happens when sutures are overtight.
Case study
A 56-year old Caucasian male presented with a recurrent basal cell carcinoma of his scalp. The lesion was incompletely removed by a general practitioner six years previously, and subsequently excised by a dermatologist twice – but recurred again. Although basal cell carcinoma may be considered a very “innocent type of cancer” because it rarely metastasizes, it is notorious for recurring locally.
The patient was then referred to a plastic and reconstructive surgeon who booked the patient for a more radical excision of the 10 x 12 mm lesion.
A couple of days later the lesion was removed under sedation in O.T with about 1 cm clean margins making the defect about 2 x 3 cm. The adjacent tissue was undermined for a reasonable distance and closed primarily with 3-0 monofilament resorbable suture material.
The wound appearance at different stages:
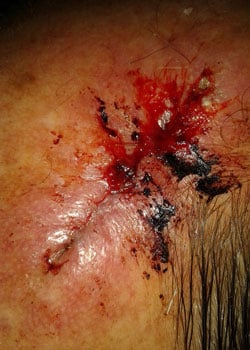
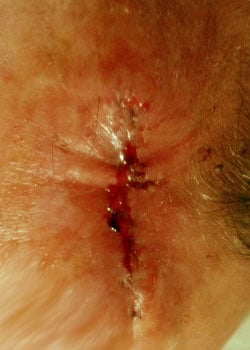
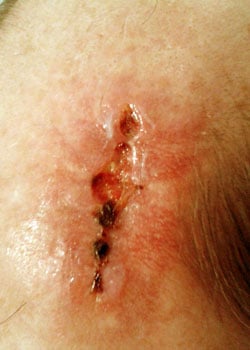
On inspection, the wound started to open up and dehisced quite severely. It was decided to allow the wound to granulate and thus heal by secondary intention.
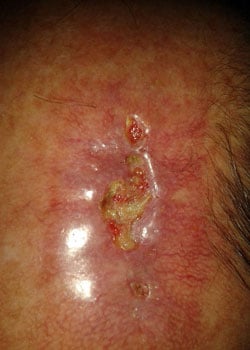
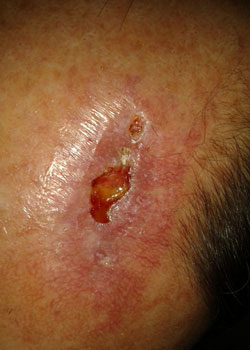
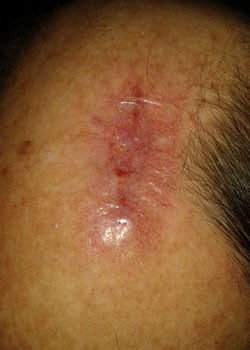
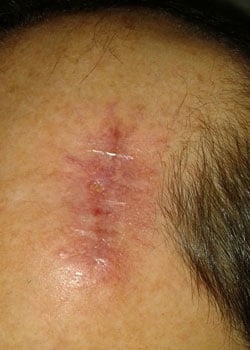
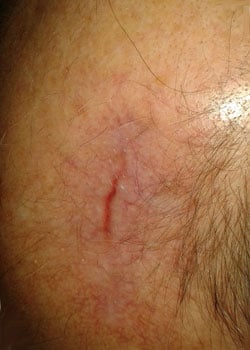
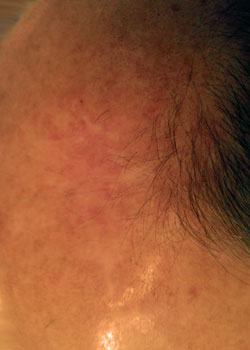
Discussion
The surgeon opted for a primary closure but may have considered using:
- A free skin graft – In my opinion, this would have given a much worse aesthetic outcome. But if the defect was anything more substantial, the surgeon may have had to use this option. Should this procedure be selected, the donor site should be kept in mind since it becomes a secondary surgical site with all the possibilities of complications developing.
- A local pedicled scalp flap – This may have been a better choice because the defect margins could be increased. This option minimizes the tension on the wound margin since it “spreads” the wound defect more evenly over a larger area.
- Alternative suture materials and techniques – The surgeon could have undermined the wound edges even more and then used a deep layer of resorbable and non-resorbable sutures on the surface for the final closure. This choice gives the surgeon control over the length of time to keep the suture in place. Vertical and/or horizontal mattress suture may have been a better suturing method to use as it would have added a bit more “hold” to the wound closure.
Retrospective wisdom is valuable because it allows for evaluation of choices made – what worked, what didn’t, and what could have been done differently. In my opinion, the surgeon achieved an acceptable and reasonable functional and cosmetic result.
Placement of sutures in an infected wound
Three goals comprise proper wound management.
- Provide for a favorable environment for hemostasis.
- Prevent any infection.
- Arrive at a scar that is aesthetically acceptable.
Infection is a crucial consideration when treating wounds, and all wounds are considered to be contaminated since underlying tissues have been exposed to outside conditions that generally thrive with bacteria. Sutures should not be applied to infected wounds. Suturing wounds is about closing the dead space between severed tissue walls so that they can undergo the natural process of hemostasis. If infected wounds are sutured, or wounds are sutured without being thoroughly cleaned and debrided, an infection will grow and spread, compromising the healing process. Therefore, any infection must be effectively treated before the sutures are applied.
Misplacement of sutures
The most common cause of wound dehiscence is placing sutures very close to the wound edges. Experimental studies show that the more distance there is between the lips of a wound and the suture, the lesser the chances of wound dehiscence. This is because the lip or edge area of the wound displays inflammatory changes, swelling, increased blood supply and reduced collagen structure. The introduction of collagen fibers during the healing phase also puts pressure on the surrounding area, thereby increasing wound tension. Finally, necrotic tissue and aponeurotic tissue zones within the area can also affect suture hold.
Adoption of incorrect suture technique
If the wrong suture technique is used, it can create wound complications such as infection, improper healing, circulation issues, or puffy, broad, or dark scars. Suture breakage is one of the most common problems when improper suture techniques are used. Breaks in sutures can occur due to inappropriate materials, irregular application angles, improper suture material or suture size, and excessive suture tension.
There are eight basic suturing techniques.
- Line of interrupted sutures.
- Running suture line.
- Running locked suture.
- Vertical mattress suture.
- Pulley stitch, type 1.
- Far-near near-far modification of vertical mattress suture, creating pulley effect.
- Horizontal mattress suture.
- Half-buried horizontal suture (tip stitch, three-point corner stitch).
Improper suture techniques can also lead to infection by allowing bacteria to enter the wound. Infection can compromise the healing process and even require that the wound be reopened for cleaning.
Removal of sutures too soon or too late
For a wound to heal properly, it must be assessed and treated correctly. This involves proper cleaning, debridement, and suturing of the wound. Part of the healing process includes applied sutures being removed at the right time which can vary depending on the stress placed on the wound and where it is located. Although the specific situation determines when sutures are removed, they are customarily taken out between 5 to 14 days. If sutures are removed too soon or are allowed to remain too long, complications may arise.
Removing sutures too soon
Sutures are applied to close a wound to keep bacteria out and to allow tissue colligation. If sutures are removed prematurely before underlying tissues have bonded sufficiently, then the wound could reopen (dehisce), damaging newly colligated tissue and allowing bacteria to enter. Deep wounds are particularly vulnerable to dehiscence if they do not have adequate absorbable sutures buried in the underlying tissues providing more tensile strength to hold the wound together.
Removing sutures too late
There are several problems which can arise from sutures being left in too long. First of all, because sutures are looped around wound edges, scar tissue can begin to form around them if they are left in too long. Also, scarring of the wound closure as well as “railroad tracks” from the sutures themselves can be excessive if the sutures remain past the prime removal time. This can be quite problematic if the laceration is in a sensitive area such as the face – therefore, in most cases, facial sutures are removed no longer than five days post-operatively.
The risk for keloid scar formation is also increased when sutures are allowed to remain for too long a period. Keloid scars consist of firm tissue that is much larger than that which forms normal scar tissue and are common occurrences in wounds of the chest, waist, shoulders, elbows, arms, and ears.
African Americans and those having a history of keloid scarring must have their wounds monitored closely so that sutures can be removed promptly to reduce keloid formation. The risk of keloid formation is also higher if the wound dehisces due to premature removal of sutures. It is difficult to be precise on timing, which is why diligently watching the healing process is vital if keloid formation is to be avoided.
The existence of foreign object in the wound
Any wound should be thoroughly cleaned and, if necessary, debrided to remove all foreign material from it. Foreign objects may include wood or metal splinters, glass shards, bone fragments, thorns, gravel, hair, cloth fibers, etc. If external items are not detected during the initial assessment, and the wound is closed, they can present problems such as bleeding, inflammation, infection, and excessive pain.
It is far better to remove all foreign materials during the initial assessment and before closing the wound because objects are more visible. Once a wound is closed with foreign material sutured inside, problems such as inflammation, granulation, infection, and scarring may occur.
Signs of embedded foreign objects
Quite often, patients can feel if a foreign object is present during the initial treatment of wounds. If this is the complaint, providing a more thorough assessment at that time may be beneficial to the patient. However, if foreign bodies are missed and remain in the wound, the following signs/symptoms will ensue:
- Local inflammation.
- Impairment of healing.
- Pain.
- Bleeding
- Bruising
- Persistent draining of an inflammatory exudate or pus.
If signs of remaining foreign objects occur after a wound has been sutured closed, the clinician may opt to use special investigations like X-rays, MRIs and CT scans to assess for the presence of foreign material remaining in the wound.
The longer the object remains in the body, the more it incorporates ingrowth of tissue. An abscess can form, and fistulas may develop between organs. The foreign body reaction may be immediate or may be delayed for years. Diagnosis is sometimes difficult and costly, and removal of the object usually requires major surgery.
Retained sponges can be removed through laparoscopic surgery if they are discovered before adhesions develop.
Determining if foreign bodies should be removed
Once a foreign body is detected, a determination is made if it should be removed at all. If more damage will occur by removing it, the decision may be to leave it in. Other times foreign objects can be removed rather easily. In other cases, the body may dissolve, absorb or expel them naturally over time.
Case study
A 45-year old male presented with vegetative material extruding from a laceration at the superior orbital rim. He had sustained a mechanical fall into a bush three months before presentation. He arrived at an outside ED, where the laceration was repaired. His exam revealed a well-healed periorbital laceration and 20/20 vision on the Snellen chart. A CT scan showed a linear foreign body with its proximal end in the medial orbit.
This object traversed the medial orbital wall, ethmoid sinus, and sphenoid sinus. A dehiscence of the posterior sphenoid sinus wall was noted adjacent to the posterior edge of the foreign body. A CT-A confirmed that there was no apparent injury to the carotid artery. Due to the risk of vascular injury, the procedure was performed in the IR suite. Given the proximity of the foreign body to the carotid artery, an angiogram and balloon occlusion test were completed before the attempted removal and a sheath was kept in place.
A combined endoscopic and open approach was performed by the ophthalmology and otolaryngology services department. A septoplasty with posterior septectomy, left total ethmoidectomy and bilateral sphenoidotomy was required to expose the object. Following this, the team was able to see a stick entering the ethmoid sinus at the lamina paprycea and extending to the right lateral sphenoid sinus. Next, a periorbital incision was made, and dissection was performed along the medial orbital wall until the stick was encountered.
The object was then able to be removed by grasping its proximal end in the orbit and pulling it out. The patient had no neurological deficits postoperatively and was discharged the following day.
Formation of a large blood clot (hematoma)
Uncommon hereditary coagulation disorders can lead to wound dehiscence. In the first month after transplantation, most infections are caused by the same hospital-acquired bacteria and fungi that infect other surgical patients (e.g., Pseudomonas sp causing pneumonia, gram-positive bacteria causing wound infections).
The most significant concern with early infection is that organisms can infect a graft or its vascular supply at suture sites, causing mycotic aneurysms or dehiscence.
Presence of arterial bleeds
When arterial bleeds exert immense pressure inside the wound, it opens. Bleeders are controlled either by ligation (typing bleeding vessels off), or diathermy (burning them closed with an electric current).
Insertion of sutures in a malignant tumor
One of the attributes of a cancerous growth is the loss of cellular adhesion. Sutures placed in a malignant tumor prevent healing.
Prevention
Wound dehiscence may be prevented by taking the following measures [2]:
- Avoid unnecessary stress or strain to wound area such as heavy lifting, exercise, vomiting, coughing, or constipation.
- Brace the body with a hand or a pillow at the wound site to relieve stress to the wound when doing an activity.
- Comply with the doctor’s post-operative instructions and prescribed medication.
- Employ wound care, dressing, cleaning and hygiene as prescribed by the doctor.
- Maintain good hydration and a healthy diet which can lead to faster healing and prevention of constipation.
Know how wounds normally heal [3]
A normal healing process after surgery can be divided into three stages.
Stage One:
- Lasts one to six days.
- There may be redness and swelling.
- The wound may feel warm and slightly painful to the touch.
Stage Two:
- Lasts four days to a month.
- A scar begins to form.
- Edges will pull together and there may be some thickening. There may also be some red bumps inside the wound site.
Stage Three:
- Lasts six months to two years, depending upon the type of surgery.
- Wound fills in and a new surface is present.
- Scarring becomes thinner, flatter, and whiter.
Any deviations from this healing process, particularly between five to ten days postoperatively, could indicate possible dehiscence. Most dehiscences occur four to fourteen days after surgery. Contact your healthcare professional if there are any concerns about the healing progression.
Be proactive and prepared
Left untreated, wound dehiscence can lead to more serious or life-threatening conditions. By understanding the healing process and being attentive to it, you’ll recognize if it’s falling outside typical parameters. Then you can get in touch with your healthcare provider for early intervention. Through this simple, proactive measure, you may avoid dehiscence and contribute to an optimal healing outcome.
References
[1] Educational Programs, MD3 Clerkship, General Principles of Knot Typing (Basics); (taken from: https://surgery.vcu.edu/education/clerkship/knotbasics.html)
[2] Dehisced Wounds, https://www.woundcarecenters.org/article/wound-types/dehisced-wounds
[3] How to Know Your Surgical Cut Is Healing Right, 2016, https://www.webmd.com/healthy-aging/surgical-incision-healing

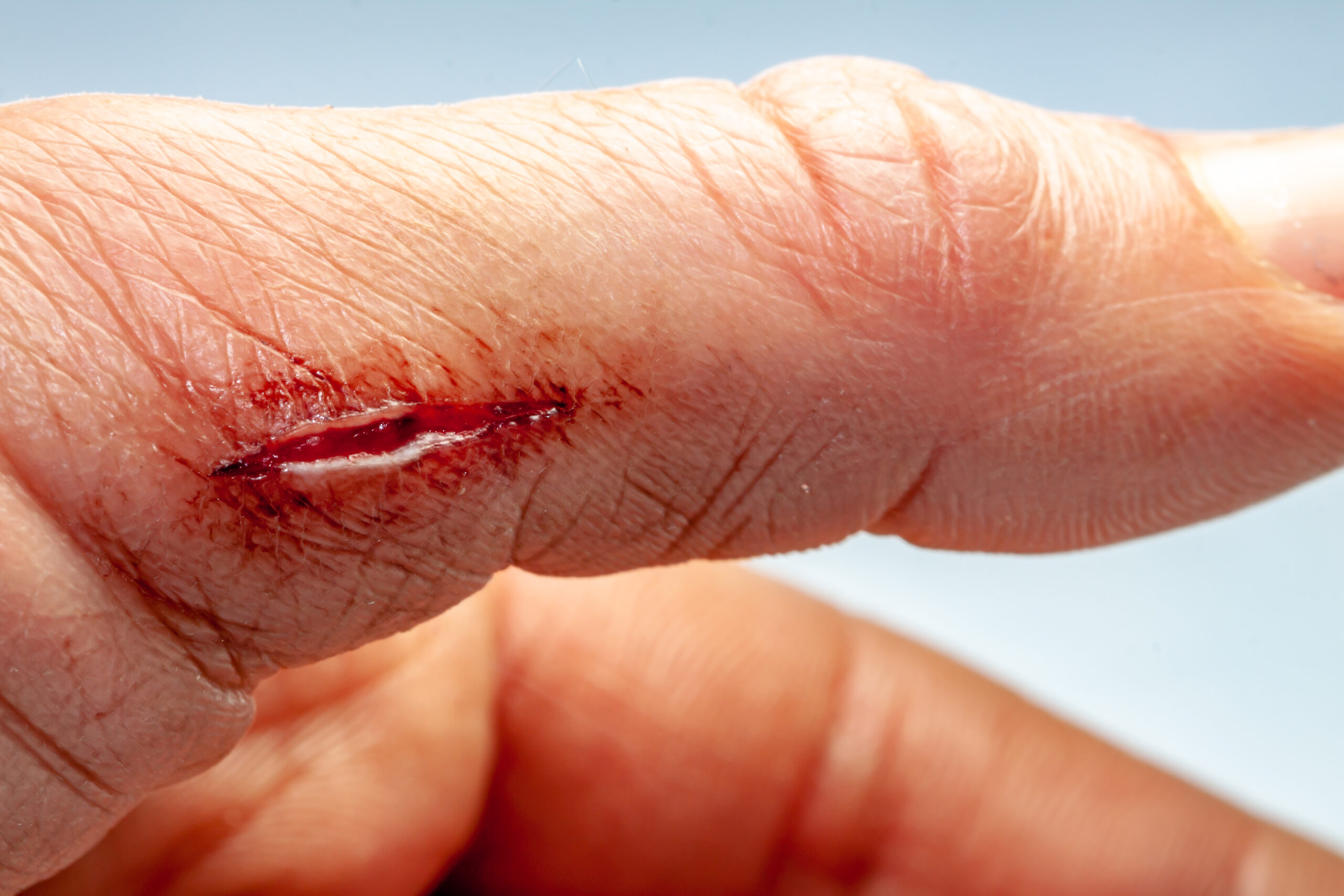
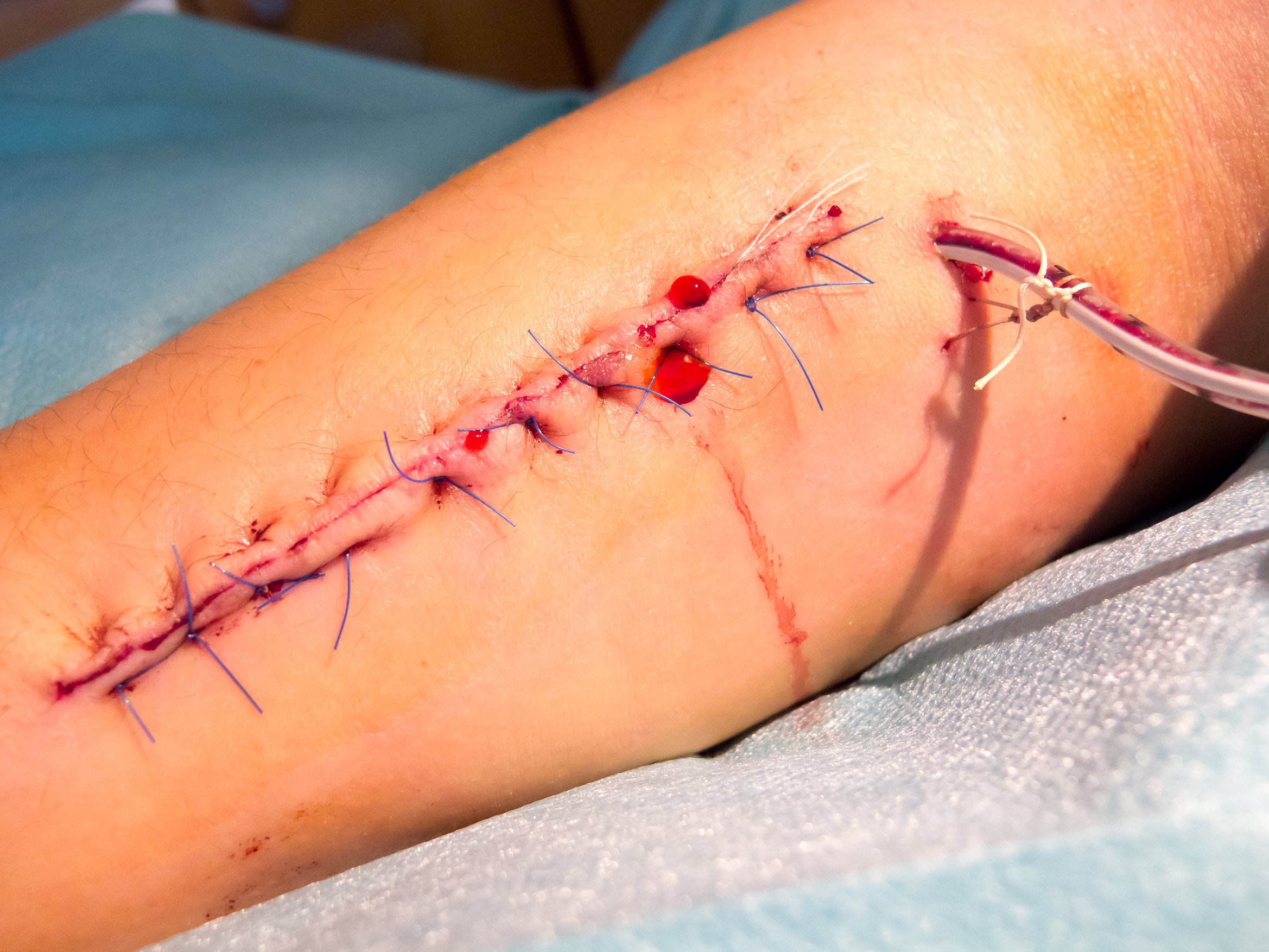
Hello and thank you for the very helpful and detailed article. I’m 5 weeks out from breast implant explantation for BII and I noticed a slight burning sensation while showering last night in the lower area of my left nipple. Upon further inspection I found a small wound about 1cm long with a tiny hole (VERY similar to the example used in your article) and it oozed a slight amount of a yellowish transparent liquid.
I spoke to my surgeon this morning and she said it could possibly be a reaction to the stitches and my body potentially trying to expel them through partial wound dehiscicion (given my BII history, I wouldn’t be surprised. I pretty much reject anything!)
I was told to keep the area dry and clean and that it would heal on its own. I also wanted to share that this was the breast that had to be operated on twice (emergency surgery the following morning) due to an issue with proper draining. I researched some of the causes and found that reopening of a wound through additional emergency surgery can increase the likelihood of getting wound dehiscence.
Anyways, thanks for the article. It brought me some peace of mind and lots of knowledge while I waited to hear from my surgeon. I just hope this one heals as nicely as the example in the pictures of your article 🙂
Trust all sorts out! 🙂
I had a suspicious lesion removed from lower eyelid, on 10th day postop it caused a dehiscence, I called plastic surgeon and they prescribed an antibiotic, said he would do surgery in three days. Surgeon never asked me to come in to examine the wound, I was forced to have a gaping hole for three days, when he seen me he apologized for making me wait so long, said may have been faulty sutures. I don’t feel I should be liable for the second surgery, I did everything was told to do. Surgeon said he had two other patients that had a similar situation, that’s why he though maybe faulty sutures. Now I have had 2 surgeries and responsible for the cost.
Sad situation – but dehiscence can happen in the best of hands (should be quite rare though).
I have just gotten an appendectomy three days ago and was told that it’s okay to shower and that I have to trim the steri-strips when they lift from the skin. After trimming the steri-strips on the incision on my belly button I was able to see inside and I realized that some water had gotten in so I used a q-tip to dry the inside and sterilize the area with hydrogen peroxide to prevent infection. The q-tip has some blood on it and I noticed that the glue holding my incision together was dissolved at the top and it seemed that the incision was opening. What do I do?
Get professional advice – meaning let your surgeon inspect the surgical wound.
I had a sebaceous cyst removed from my upper back, in a tough spot. No bleeding after 4 days, but then at 8 days it opened up. Went back and had an extra superficial stitch put in at 10 days. Bleeding is slowly decreasing (changing non-stick pad once per day now) now at day 15. Not painful, just a bit tender.
Doctor says keep doing the wound care…is this relatively normal in this area (upper back, directly below shoulder blade)?
I have to admit that this is one of the dissidence prone areas – just keep on following orders and nurse the wound back to health.
I’ve had 2 spine fusions 3 infections with debridment due to the spine fusions and then removal of hardware. Now 5 years later my skin is so thin back there I felt a watery subsense back there and it was bleeding and ooozy with a split in the scar. It is red around it…should I leave it and try and to tend to it myself or should I comment to my doctor about it. It is painful to the touch and to lay on it.
Sounds like all the classical signs of infection – see your doctor.
I have had multiple surgeries on my foot and ankle, to include but not limited subtalar fusion, joint debridement, scar tissue removal from ligaments and tendons, a strayer procedure and the last being a TAR. After the last surgery and the one before it, I have dark areas with a blueish tint to the skin on large areas om my foot and ankle, mostly around the incision sites. My surgeon reassures me that everything is fine and it is not uncommon to happen. He stated it’s similar to freckling on the skin. I have had some of it for going on 4 years now, Have you heard of this? What is it called and what causes it.
It is called post-inflammatory (post-traumatic) hyperpigmentation and is actually fairly common.
I have been looking for advice with regard to my 3year post op orif ankle. The site opened up and to make a long story short, it has been three years in September, and still it has a pus like exudate coming from it. I did go to wound care after the surgery, however I had to discontinue due to lack of insurance. It has closed, and I have to make a small opening to get the fluid out, it is painful if I don’t.
You probably will need to have an orthopod look at it – and possibly remove the “hardware”
How can i be sure that all stitches have been removed ? Is there any way to detect if any stitches left over ?
There is really no good way – apart from trusting the medical professional removing the stitches. Even in best of hands a stitch fragment may stay behind and may or may not fester out of the wound.
Dermatologist removed a cyst just below my left earlobe. 5 days later the incision is leaking/weeping bright red thick blood. 3-4 dressing changes per day is not helping with the bleeding. Dermatologist is suggesting that a blood vessel has been nicked and wants to reopen wound for blood vessel repair. Is this best done in a hospital or is it ok in the dermatologist office?
Sounds like an office procedure to me. But will go by the dermatologist’s judgement 🙂
Dr. I appreciate your reply (above). Had 2nd surgery 4 weeks ago….. debridement of wound on elbow with artificial skin graft. It has failed. Wound is now so wide, black and painful. Seeing a plastic surgeon for consult. I’m so scared because pain gets worse everyday. Have you heard of having reconstructive plastic surgery due to wound not healing? thank you.
I had a scar revision on my face(right cheek bone area), I have an appointment to remove the stitches 12 days later. Is that too long for stitches to be on face area? I’m concerned, as you article said stitches on face should be removed within 5 days. Please help I’m at day 9.
It depends on what type of suture material, the suturing method and another couple of variables. If the surgeon used subcuticular suturing – 12 days is fine…
Interrupted sutures – one should try to get out in 4-5 days (if possible)
Over 35 years of looking at dehisced wounds I have never seen a broken suture from a simple stitch, or an untied or loose knot from a simple stitch. Whether square or other knots were used, there were often enough knots tied to assure the knot stayed intact without loosening of the inititial knots holding the simple stitch together…
The few broken sutures or knots causing dehiscence of a wound or anastomosis were from continuous stitches in running closures…
The testing of knots (and sutures) has been endless since Taylor’s 1938 paper: https://www.ncbi.nlm.nih.gov/pubmed/17857148…
More at: https://www.ncbi.nlm.nih.gov/pubmed/17324776…
This is an interesting comment – and I won’t just swallow hook and all – but there is definitely some truth in it. An interrupted suture is very much a predictable suture to use, as opposed to a continuous suture – if it gets undone – the totality of the wound opens up. I have to say that certain types of suture materials – especially the mono-filaments like Monocryl has a strong tendency to unravel and is certainly to some extent dependent on good knot tying techniques. Thank you for the references – jewels from the past! Thought provoking – any other comments from experienced surgeons?
I had a pilonidal cyst surgery two months ago, the upper part of the wound (where the cyst was) was not closed with stitches, whereas the lower part (about 6 cm) was closed with stitches. Two weeks post surgery my doctor removed these stitches and everything was ok. But 2 weeks after removing them the lower wound reopened. After carefully taking care of it and applying some medicine on it (betadine ointment) it closed again and one week later opened again then closed for about 3 weeks. After this period of time i went on holiday and the lower wound reopened due to a lot of swimming and movement and then 1 week later after applying medicine it closed. Today ( 1 week from recovering) a small part of the wound opened again, i want to see what should i do. Does anyone have any idea of what is happening to me? And why?
I am sorry to hear this is happening to you. I am unable to provide medical advice, but suggest you see your doctor.
About a month ago I had an appendectomy everything was fine everything looked as if it was healing fine. Then a few days ago my wife noticed it was red and puffy then the next day it looked as if it had a hole and looked as if it full of puss and put a hot compress on it and sure enough it was. I call the Surgeon 4 times due to an auto ammun issue I have and he never called back well needless to say it is getting worse by the day I now have three holes with puss and looks as if a fourth could happen and it all red in the area it is tender to the touch why could this be. I just started humera also my wife is besides herself I called my family dr they told me to call the surgeon?????
I am sorry this is happening to you. It sounds like it may be a serious situation. I can’t comment on what this could be or give any medical advice. The best thing I can tell you is to call your surgeon or go to an emergency room.
I shattered my elbow in a fall and had 3 plates and 21 screws. wound area was black and surgeon was watching it. finally wound care dr. shone a light and saw hardware showing. was sent right back to surgeon who didn’t see it. i had to tell him to shine light on blackened skin. he saw it and scheduled me for in-patient debridement surgery (under general anesthesia) monday. i’m scared there’s not enough healthy skin. i’m in pain. hand is swollen and half numb. how common is this? i am terrified.
Not too uncommon – but your surgeon seems to be very much on top of things. Always feel free to get a second opinion if you are unsure…
Hi
I had an excision of a bcc on my right temple. Nice looking stitches, taken out one week later and looked fine but wound opened up overnight while sleeping. Site doesn’t look red. Will steri-stripping it help? Presume I should see dr for antibiotics. Thanks for any advice
I’m sorry to hear this has happened. I cannot dispense medical advice, but can recommend you see the doctor.
I had 7 moles surgically removed from my face 10 weeks ago. Healing was great and scarring almost un noticeable. 2 days ago 2 of the incision sites turned black and started to bleed and now I have 2 holes in my face. Why would this happen 10 weeks post op? No swelling. No redness. No concern at all during healing process.
Possibly deep hematomas? Get professional advice as soon as feasible!
Post op 5 weeks from breast reduction and I kept complaining about the pain and fevers I had. Left side had the cut underneath that looked infected and not healing. Right side looked amazing. Week 3 had two fluid pockets, drained still fevers admitted for antibiotics for several days and now week 5 and left side is now bigger and longer and wider then ever and when I take off the dressing there is green discharge with the cream. Dr says its fine! I say its not. Could my wound be worse on the inside?
I am sorry to hear you’re having this kind of difficulty. I cannot give you a medical opinion on a website. But based on what you have shared, my non-medical opinion is that you get a second opinion on what might be happening. That is the best I can offer in this venue.
Recently had ankle surgery requiring an incision on top of the ankle. At 2 week appointment, doctor decided to leave stitches in for another week as there was an area of ‘concern’ in the incision. The stitches were removed a week later and the area of concern opened up. Although I have limited my activity and weight bearing the incision has now opened to half its original length and we’re treating with Silver Sulfadiazine, twice a day with re-wrap, vitamin C, a multi-vitamin and antibiotics for good measure. The wound looks no better or worse and in it’s location I’m wondering how it can ever close. Any ideas?
This is a not too uncommon complication with surgery below the knee – and at the end of the day one need to leave it to natural healing mechanisms – if excessive scarring – cortisone injections in scar tissue/cortisone creams and physiotherapy (if limited function/movement) – not an ideal situation…
Interesting article. I’m wondering about dehiscence in a very old wound – 22 years ago, I received 3-4 stitches to close a cut on the tip of my thumb. It appeared to heal nicely, but in recent years when the weather is cold and dry, skin splits at my scar. Sometimes it splits enough to ooze a little blood and throb a bit. It always heals again when the weather improves and I moisturize the area. Is there a way I can get this wound to heal permanently?
The short answer is- not really – it is a case of do it first time properly!
Is it possible to have wound dehiscence internally only? Externally the incision is intact except an area of a scab that’s still healing. I went through a major surgery on my back to reattach muscles to my scapula. I had 22 staples. 2 days post op I vomited violently and felt terrible pain in the inferior area of the incision. I happened to be at the dr’s office and he assured me it was just post op pain. I continued having pain here with every movement. After 4 weeks in a bolster sling, I was told to discontinue wearing it. At that time I literally felt like someone was unzipping my scapula off of my back. It swelled and discolored. No signs of infection…oozing or fever but I couldn’t stand for it to be touched in that area(still can hardly stand it actually at 18weeks post op). I have had my pain management dr, my pcp and my surgeon look at it but they reassure me the incision looks fine. It doesn’t feel fine though. I know looks can be deceiving. To complicate things….I am a lupus patient and try to reiterate to them that I heal very slowly and differently than other people. Please help if you can offer any advice. I have lots of pics of this area along my course of healing….something just doesn’t seem/feel right. Thank you for your time.
The short answer is – yes – one can get wound dehiscence in the internal layers with or without surface dehiscence – especially with muscle that moves and contracts all the time! Trust it helps – and best with your shoulder!
P.S. A MRI scan will show if it is fine…or not.
Thank you for the reassurance. Although, I’m sure we will never know if I have had it or not because my MRI that was just done showed fluid and possible retear but I’m being told this is normal to be seen post operatively…..18weeks seems like pretty far out to still have fluid and be in this much pain but obviously I’m not the experts. Just know my body pretty well and somethings not “sitting right” in my gut. I know what you mean by trust but who do I trust….my drs or my gut. At this point I guess it doesn’t really matter. But thank you for the response and well wishes!